Hospital Value
Hospital Value:
With a downward trend for healthcare reimbursement1 coupled with a high expected TKA procedure growth rate,2 hospital economics are driving the need to improve OR efficiencies.
Not only are costs driven from the procedure itself, but patient care after surgery is costly and increases significantly with complications. (Figure 1)
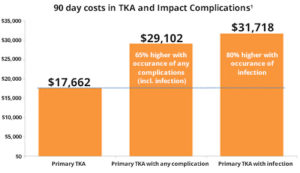
What are some of the main cost drivers that can be improved today?
- The average TKA procedure with an off-the-shelf implant system takes about 100 minutes4 and it can take about 33 minutes to turnover an OR.5-7 At an average cost of $40 per minute, operative and turnover time costs can contribute to almost a third of the total cost of the procedure.
- Off-the-shelf TKA implants with standard instruments typically require a minimum of 6 instrument trays,8-11 which comes with an average cost of $58.18 to prepare and sterilize each tray.8 In addition, studies have found the rate of compromised trays to be as high as 16%,9 requiring additional sterilization and cost to the hospital.
- Patient care after surgery is widely variable and adds considerably to the overall cost related to the procedure. Cost is influenced by length of hospital stay, post acute care treatment options, and adverse events associated with the surgery.
In the operating room, less is more
One benefit of a fully patient-specific model is the ability to deliver everything for surgery in one box, with only one tray of reusable instruments.
The benefit of patient-specific instruments can also extend to operative time. Studies using patient-specific instruments with off-the-shelf implants have shown a savings of as much as 15 minutes of operative time.13-15
A full set of pre-sterilized instruments also reduces the amount of instrument tray sterilization that must take place. Instead of sterilizing 6 or more trays, only one tray is required for an iTotal® procedure.
It pays to get patients back on their feet faster
Recovery from surgery can take a few different forms and is often impacted by certain clinical outcomes. Post-operative care can add significantly to the overall procedure cost.
For example, the economic impact of blood transfusions can be very costly. Blood transfusions have been associated with $2,237 increase in admission costs, as well as an increased risk of infection and other complications.16
The factor that has the most potential to drive up cost, however, is post acute care. One study that looked at the average costs across different discharge scenarios found that care in a rehab facility averaged over $16,000.17
In one study, the customized iTotal® demonstrated advantages compared to standard off-the-shelf implant systems, including:
- More patients discharged in under 3 days (42% vs. 30%)
- Lower rates of blood transfusion (2% vs. 11%)
- Fewer patients discharged to a rehab facility (27% vs. 37%)
- A lower overall incidence of adverse events (10% vs. 44%)18
- Weiner, et al; Population aging in the United States of America: Implications for public programmes. International Journal of Epidemiology; 2002, 31: 776-781
- Kurtz, et al; Projections of Primary and Revision Hip and Knee Arthroplasty in the United States from 2005 to 2030. Journal of Bone and Joint Surgery; 2007, 89: 780-785
- Kremmers, et al; Determinations of Direct Medical Costs in Primary Total Knee Arthroplasty. Clinical Orthopaedics and Related Research; 2013, 471: 206-214
- Ho, et al; Are Critical Pathways and Implant Standardization Programs Effective in Reducing Costs in Total Knee Replacement Operations?; Journal of the American College of Surgeons; 2007; V205(N1): 97-100
- Lionberger, et al.; Custom cutting jigs improve OR efficiency, but not accuracy; Proceedings from 21st annual AAHKS meeting; Nov 2011: Paper #33
- Cima; Use of Lean and Six Sigma Methodology to Improve Operating Room Efficiency in a High-Volume Tertiary-Care Academic Medical Center; Journal of the American College of Surgeons; 2011; V213:pp.83–94
- Attarian, et al; Developing a High-efficiency Operating Room for Total Joint Arthroplasty in an Academic Setting; Clinical Orthopaedics and Related Research. 2012
- Watters, et al; Analysis of procedure-related costs and proposed benefits of using patient-specific approach in total knee arthroplasty; Journal of Surgical Orthopaedic Advances; 2011 ;V20: 112–116
- Mont; Single-use instrumentation, cutting blocks, and trials decrease contamination during total knee arthroplasty: Journal of Knee Surgery; 2012
- Bonutti, et al; The use of disposable cutting blocks and trials for primary total knee arthroplasty; Techniques in Knee Surgery; 2010; V9(4): 249-255
- Johnson, et al; The benefits of customized patient instrumentation to lower-volume joint replacement surgeons: results from practice; American Journal of Orthopedics; 2011; V40(11 Suppl): 13–16
- Takeuchi; Technical Report: Disposable Laparoscopic Surgical Instruments and the Economic Effects of Repackaging; Journal of Laparoendoscopic & Advanced Surgical Techniques; Apr 2005; V15(N2): 176-181
- Barrack, et al; Patient specific cutting blocks are currently of no proven value; Journal of Bone & Joint Surgery; Nov 2012; V94B: Suppl A; 95-98
- McQueen, et al; The Effect of Single Use Instrumentation on OR Efficiency for Total Knee Arthroplasty: A Multicenter Efficiency Study. Poster Abstract, AORN Congress, 2009
- Nunley; Are Patient-specific Cutting Blocks Cost-effective for Total Knee Arthroplasty?; Clinical Orthopaedics and Related Research; 2012; V470: 889–894
- Szubski, et al; National Trends in Utilization and Outcomes of Allogenic Blood Transfusion in Primary Total Knee Arthroplasty: A Prospective Comparison of Navigated and Nonnavigated Cases. Journal of Knee Surgery; 2013, Vol. 26: 285-290
- Ramos, et al; Correlation Between Physician Specific Discharge Costs, LOS, and 30-Day Readmission Rates: An Analysis of 1,831 cases. Journal of Arthroplasty; 2014, 29 #4: 674-677
- Culler, et al; Hospital Outcomes and Cost for Patients Undergoing a Customized Individually Made TKA vs. Off-The-Shelf TKA. ICJR Pan Pacific Annual Meeting 2014, Abstract #O18A3
About Conformis
We start with a simple idea: make the implant fit the patient rather than force the patient to fit the implant
About ConformisHealthcare Professionals
Resources and information for medical professionals
Healthcare Professionals


 FAST TRACK HOSPITAL METRICS & PATIENT OUTCOMES
FAST TRACK HOSPITAL METRICS & PATIENT OUTCOMES